|
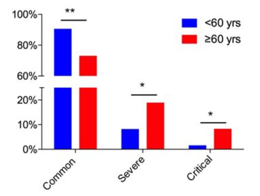
Why does the elderly face a higher mortality rate with COVID-19? introduction For almost half a year now, COVID-19 has dramatically changed our daily routines, whether that be switching to getting groceries delivered to our front doorsteps to choosing outdoor seating at a new restaurant. In my family, we are very careful about meeting with anyone outside of our immediate home because we don’t want to risk the health of my immunocompromised family members. Instead of going in to work, my mom chose to telecommunicate with her patients. Instead of buying groceries every week, we’ve changed all of our recipes so that we can only buy things once a month. All of these changes terrified me at first until I talked to my older relatives and recognized all of the precautions they had to take as well. With this in mind, I started wondering why certain people’s immune system, specifically the elderly, are more susceptible to COVID-19 and severe complications from the disease. In this article, I will discuss how aging affects the immune system and why that is a key player in the high elderly mortality rates with COVID-19. How does our immune system work? Our immune system identifies dangerous things that can hurt us and mounts protective defenses to neutralize the threats. Certain cells in our body have specialized receptors that can sense different features on an invader (like harmful viruses.) For instance, the family of receptors known as Toll-like receptors (TLRs) can sense viral RNA (Mueller, McNamara and SinClair). Once these specialized cells recognize a foreign object, it incites a cascade of events. The cycle begins with inflammation in which chemicals and cytokines, proteins that cause the recruitment of other immune cells, are released. After this siren call, certain immune cells, like B and T cells, will replicate. Finally, antibodies or specialized T cells are produced to kill the foreign invader. However, the immune system and its functions can be altered by different factors like our age, sex, and/or prior exposure to different diseases. How does the immune system decline with age? Immunosenescence is a new concept in immunology that focuses on understanding how our immune system declines as we age age. As a whole, aging decreases our immune system’s overall effectiveness and limits its ability to serve as a pathogen alert system. For instance, the thymus, an important organ where T cells go to mature, is a victim to immunosenescence. With age, the thymus physically shrinks which decreases the amount of mature T cells being produced in our bodies. With fewer mature T cells, the body can’t effectively respond to disease-causing pathogens thus allowing easier entry for viruses like COVID-19 (Kadambari, Klenerman and Pollard). Since the immune system is the body’s first defense against COVID-19, weaker immune systems could correlate with more severe cases of this dangerous disease. How does immunosenescence impact COVID-19 severity? COVID-19 is a disease caused by the SARS-CoV-2 virus that infects individuals through the ACE-2 receptor, a receptor found throughout the body. Sadly, 74% of fatal cases of COVID-19 are in patients aged 65 and above, suggesting age may play a significant role in COVID-19 severity (See Figure 1). In most cases, mortality is caused by organ failure stemming from excessive inflammation that occurs in a phenomenon known as cytokine storms (Viana, Nunes and Reis). Cytokine storms are when immune cells produce excessive amounts of pro-inflammatory proteins, known as cytokines, that trigger excess inflammation in major tissues and organs. Notably, 82% of elderly patients suffering from a cytokine storm succumbed to the disease (See Figure 2). While many factors are being studied as to how these storms are triggered, the top suspect is pre-existing inflammation caused by immunosenescence or gut dysbiosis (Mueller, McNamara and SinClair). Thus, older patients are naturally at risk for poorer outcomes of COVID-19. Possible Solutions To prevent the elderly from facing harsher cases of COVID-19 through the immune system and gut health, scientists are looking at a myriad of possible therapeutics. To target the aging immune system, geroprotectors could be utilized. Geroprotectors are molecules that target aging by regulating cellular metabolism and controlling certain immune factors, such as the production of cytokines (Mueller, McNamara and SinClair). By controlling these key functions, Geroprotectors could prevent an uncontrolled cytokine storm and promote healthy immunoreactions to the SARS-CoV-2 virus. As we talked about in my first article, the ACE-2 receptor plays a role in gut homeostasis and is targeted by the SARS-CoV-2 virus. Interestingly, the ACE-2 receptor’s protective functions from the SARS-CoV-2 virus are also suppressed with age, worsening gut dysbiosis and the severity of the disease. To target this and intestinal inflammation caused by the virus, soluble ACE2 or treatments to upregulate ACE2 expression may be utilized (Viana, Nunes and Reis). Finally, prebiotics or probiotics could be used to prevent intestinal inflammation or leakage since the gut microbiota also changes with age. Prebiotics are substrates that are selectively used by microbes in order to increase health. For example, certain prebiotics might shift the microbiota community in order to increase the population of good bacteria that are less inflammatory. Whereas probiotics are bacterial species that are ingested in order to shift the community towards a less inflammatory state or are ingested so that they can produce anti-inflammatory molecules (Viana, Nunes and Reis). ConclusioN As COVID-19 continues to spread across the world, scientists and doctors are rushing to find different avenues to not only prevent infections from happening, but also reduce the severity and risk of complications for those who contract the disease. Unfortunately, our elderly are predisposed to suffering complications from the disease and are most likely to wind up in hospitals and on ventilators. This may be due to numerous factors, including immunosenescence. By treating the aging immune system and preventing other issues such as gut dysbiosis, we might be able to better treat the elderly. BibliographyKadambari, Seilesh, Paul Klenerman and Andrew J. Pollard. Why the elderly appear to be more severly affected by COVID-19: The potential role of immunosenescence and CMV." Wiley (2020). Review. Liu, Yang, et al. "Association between ages and clinical characteristics and outcomes of coronavirus disease 2019." European Respiratory Journal (2020). Research. Mueller, Amber L., Maeve S. McNamara and David A. SinClair. "Why does COVID-19 disproportionately affect older people?" AGING 12.10 (2020). Viana, Sofia D., Sara Nunes and Flavio Reis. "ACE2 imbalance as a key player for the poor outcomes in COVID-19 patients with age-related comorbidities - role of gut microbiota dysbiosis." Ageing Research Reviews (2020). Review.
This content is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition.
9 Comments
|
AuthorMy name is Sarah Mathew and I was a junior in high school when this pandemic hit. I wanted to help my community in the best way I knew how: writing. Archives
December 2020
Categories |
||||||||||||||||||||||||
 RSS Feed
RSS Feed
