|
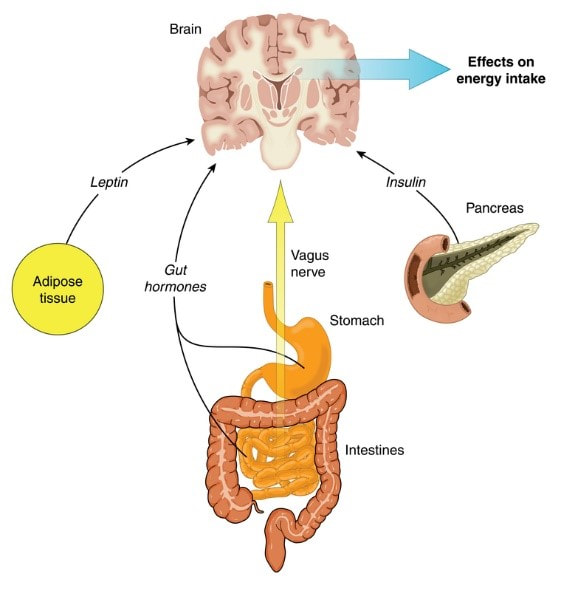
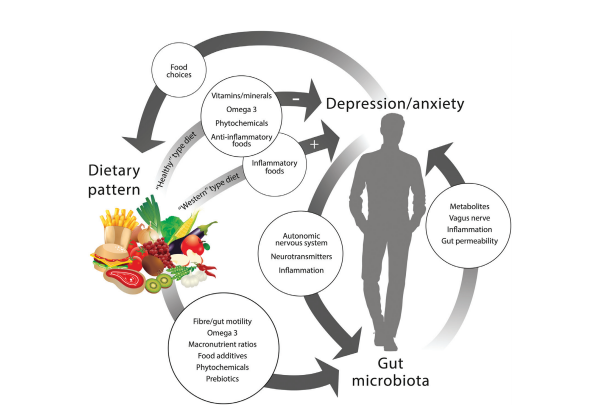
Does the food we eat affect our mental health? INtroduction We grow up not only learning from our teachers about depression and anxiety but also witnessing how it can affect the people we love. Whether that knowledge started from a Google slides presentation in health class or watching our loved one’s mental health suffer, we have all had to learn how to support each other. From this first-hand knowledge, I grew curious about the different factors that affect depression and how much of this disease is in our control. In this article, I will discuss the relationship between gut microbiota and depression, and how depression could be treated through dietary changes. What is depression? Depression is a long-term relapsing mood disorder that incites feelings of sadness or apathy. It can lead to anxiety, unexplained physical problems like headaches, and overall exhaustion (Cui). The disorder can stem from numerous causes including family history of depression, difficult stressful experiences (like abuse or the death of a loved one), or even a lack of sunlight (like in the winter months). Biologically, depression causes nerve signals to travel increasingly slow and modulates important chemicals like serotonin and cortisol. It also pushes the hypothalamic-pituitary-adrenocortical (HPA) axis activity, which oversees the bodies stress response, into overdrive (Bear, Dalziel and Coad). Microbiota interactions with the brain One influence that is gaining considerable interest involves studying how the microbiota impacts our mental health. Recent studies have found that the microbiota plays a crucial role in influencing our brain chemistry and stress response in numerous ways including vagal nerve stimulation. The vagal nerve is a system of nerves that carries signals from our digestive system to the brain and back. It’s considered to be part of our central nervous system that oversees immune response, digestion, and even our heart rate. Our vagal nerve also modulates the nutrients we take from our food consumption, which effects our overall energy intake (See Figure 1). New findings have displayed that our vagal system can “sense [the] microbiota” and that stimulation of these nerves can have a tremendous impact on our overall mood (Breit, Kupferberg and Rogler). Since the vagal nerve affects our energy levels and our mood, it could also affect our emotional well-being. The feelings of sadness or apathy associated with depression could be explained by specific signals from our vagal nerve. The intestinal microbiota performs many functions for us, including metabolizing the food we eat and the production of various vitamins and molecules that we need. Interestingly, some of these molecules directly influence our brain by connecting our emotional centers of the brain with intestinal functions, making up the gut-brain axis (Carabotti, Scirocco and Maselli). Certain bacterial species, for example, can produce local neurotransmitters such as melatonin (which modulates the sleep-wake cycle), serotonin (which modulates mood), and dopamine (which modulates motivation), that are essential for our emotional well-being (Evrensel and Ceylan). Accordingly, dysbiosis in the microbiota can have a profound impact on the gut-brain axis. Dysbiosis is when the microbiota is in a communal state that leads to excess inflammation in the gut. This inflammation is marked by a systemic increase in pro-inflammatory cytokines and increased intestinal permeability. Once systemic, these molecules can increase the permeability of the blood-brain barrier, which in turn, can stimulate parts of the brain into releasing cortisol, a known stress hormone (Clapp, Aurora and Herrera). As mentioned before, taxing situations and stress within the body can trigger depressive states. Thus, dysbiosis in the gut may lead to the incidence of depression. What is the solution? Considering the connection between the gut and the brain, novel methods of treating depression through diet are being studied. While the diet-microbiota field is relatively new, some researchers have found links between different diets and varied composition of the microbiota. For example, Western dietary patterns were found to promote gut dysbiosis and were associated with an increased prevalence in depression (See Figure 2). In a recent study, Western dietary practices predicted 39.8% of total depression incidence (Lang, Beglinger and Schweinfurth). Interestingly, on the other spectrum, adherence to a Mediterranean diet was shown to reduce inflammatory/pathogenic bacteria levels in the gut, while increasing the abundance of beneficial commensal species, which may in turn decreased inflammation (See Figure 2). Although the researchers did not specifically test for depression, these changes in the gut microbiota might be associated with decreased onset of depression. Additionally, vegetarian or plant-based diets reduce gut inflammation, promoting healthy gut interactions with the brain and possibly lessening the risk for the onset of depression (Bear, Dalziel and Coad). Conclusion Depression is a complex disease that is caused by many factors, including our intestinal microbiota. Diet may be one area that can help treat depression by influencing the composition of the gut microbiota and therefore the gut-brain axis. Diets that skew the microbiota into a healthy, and less inflammatory state, may lead to the production of crucial molecules (such as serotonin and melatonin) that can help us against the disease. BibliographyBear, Tracey LK, et al. "The Role of the Gut Microbiota in Dietary Interventions for Depression and Anxiety." Advanced Nutrition (2020). Article. Breit, Sigrid, et al. "Vagus Nerve as a Modulator of the Brain-Gut Axis in Psychiatric and Inflammatory Disorders." Frontiers in Psychiatry (2018). Review. Carabotti, Marilia, et al. "The gut-brain axis: interactions between enteric microbiota, central and enteric nervous systems." Annals of Gastroenterology (2015). Review. Clapp, Megan, et al. "Gut microbiota's effect on mental health: the gut-brain axis." Clinics and Practice (2017). Article. Cui, Ranji. "A systematic review of depression." Current Nueropharmacology 13.4 (2015). Editorial. Driver, Kate. Leaky gut and the gut brain connection. 16 September 2016. Blog Article. 24 August 2020. Evrensel, Alper and Emin Mehmet Ceylan. "The Gut-Brain Axis: The Missing Link in Depression." Clinical Psychopharmacology and Nueroscience (2015). Review. Lang, Undine E., et al. "Nutritional Aspects of Depression." Cellular Physiology and Biochemistry (2015). Review.
This content is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition.
6 Comments
Hannah
12/23/2020 07:08:04 pm
Mediterranean diet, here I come!!
Reply
Amaan N Bhimani
12/23/2020 07:13:52 pm
This was very interesting and eye-opening! The mentioning of the Mediterranean diet is an interesting point as it definitely lines up with the many other benefits often associated with it. I appreciate the inclusion of sources as it really helps to solidify this article.
Reply
Roshini
12/23/2020 07:44:03 pm
That was very informative and concise! I didn’t know that microbiota is a factor that could help create depression. Loved this!!
Reply
Aarushi Khanna
12/23/2020 07:54:56 pm
I love this read!! It’s so informative and really gives a wonderful insight on the topic!!!
Reply
Khang
12/23/2020 08:08:40 pm
Very interesting and enjoyable read. Never thought I’d be so zealous over an article!!
Reply
Elizabeth
12/24/2020 04:37:07 am
Article makes a convincing point regarding increasing the content of plant-based intake in the diet. Thank you for posting!
Reply
Leave a Reply. |
AuthorMy name is Sarah Mathew and I was a junior in high school when this pandemic hit. I wanted to help my community in the best way I knew how: writing. Archives
December 2020
Categories |
||||||||||||||||||||||||||||||
 RSS Feed
RSS Feed
